 Obsessive Compulsive Disorder (OCD) is comprised of two parts: obsessions and compulsions. Obsessions are thoughts and compulsions are behaviors. OCD is classified as an anxiety disorder because it is generally driven by anxiety. Obsessions are unwanted, intrusive thoughts that cause a person distress. Compulsions are behaviors in which a person engages to reduce the anxiety caused by the obsessions. Common compulsions that the general public is familiar with include when people will engage in checking behaviors and cleaning behaviors. The variations of presentation of OCD are quite extensive and not the focus of this blog entry. But whatever the presentation, OCD can be a debilitating condition. Some of the more effective treatments for OCD historically has been exposure therapy and cognitive behavioral therapy. Medications, especially selective serotonin reuptake inhibitors and tricyclic antidepressants, are generally most effective for OCD. But medication is not able to help all cases. Additionally, medications can have unwanted side effects. Some people refuse to engage on exposure therapy because it is by definition unpleasant. 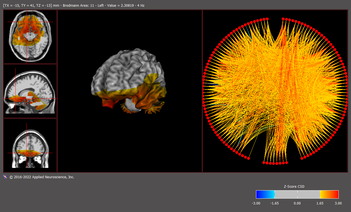 Brain image of a patient with OCD who has elevated activity in various locations in the brain related to OCD symptoms. Brain image of a patient with OCD who has elevated activity in various locations in the brain related to OCD symptoms. Neurofeedback offers another treatment for OCD which can be very effective in treating all components of OCD including anxiety, obsessions and compulsions. In my office, a brain map (also known as qEEG analysis) is conducted to identify areas of the brain that have been found in research to relate to OCD. Areas of the brain frequently found dysregulated include the cingulate gyrus, anterior cingulate gyrus and orbitofrontal cortex (Brodmann area 11). Other regions can be involved including other parts of the frontal cortex, insula and the amygdala, which drives anxiety. I almost always find excessive theta wave activity in the anterior cingulate in patients with OCD. After identifying which specific areas of the brain are dysregulated, Neurofeedback can be done to retrain these areas of the brain linked to OCD symptoms. Patients then report improvement in OCD symptoms. I do additional testing such as the Yale-Brown Obsessive Compulsive Scale (Y-BOCS) to get baseline measures of function and then track improvement. When Y-BOCS scores are normalized, treatment stops. I then track patients over a period of 6 weeks to see if scores remain normalized. In all the cases of OCD I have treated, the improvements made are permanent and no other therapy is needed. Some research has been done on OCD and Neurofeedback. Articles are listed below. If you or someone you know suffers from OCD, help is out there. Please contact my office in Palm Harbor, Florida and schedule an appointment.
0 Comments
Leave a Reply. |
AuthorI'm a Chiropractic Physician, Psychotherapist and researcher. I'm interested in helping people live their lives to their full potential. That could be simply without pain. Or it could be without more complicated physical or mental health problems. Or it could be getting help in making changes in their life so that they can achieve their dreams. Archives
June 2023
Categories |
 RSS Feed
RSS Feed